Beyond the Hype: The Surprising Truth About New Alzheimer’s Drugs (and What Actually Works)For millions of families, the fear of cognitive decline is a shadow that looms over every misplaced key or forgotten name. When "breakthrough" Alzheimer’s drugs hit the headlines, they are greeted with a desperation that fuels a multi-billion-dollar industry. But an investigative look at the high-level data reveals a stark reality: we are spending billions for single-digit returns.The gap between pharmaceutical marketing and clinical reality has reached a breaking point. While the public is sold a vision of a cure, the "gold standard" sources of medical evidence—the Cochrane Library and the 2024 Lancet Commission—reveal a different story. As we navigate this billion-dollar question, we must ask why we are willing to pay for high-risk, low-reward infusions while insurance refuses to cover the lifestyle optimizations that actually move the needle.1. The "Breakthrough" Benefits are Mathematically TrivialThe Cochrane Library, arguably the most prestigious and trusted body for evidence-based assessment, recently released a meta-analysis of amyloid-beta-targeting monoclonal antibodies, including the much-hyped Leqembi and Kisunla. The findings were so sobering they were met with immediate, heavy criticism from the drug industry and Alzheimer’s advocacy groups.The data reveals that the "breakthrough" is more of a crawl. In an analysis of 17 randomized controlled trials, the reduction in cognitive decline was often in the single digits. While the industry argued the results were skewed because the analysis included older, failed drugs, even the most "positive" individual studies only show a marginal slowing of decline. These drugs do not stop the disease, and they certainly do not reverse it; they merely slow the inevitable at an astronomical cost."The devil is in the details... the benefit is marginal at best." — Dr. Misha Kogan2. The 10% Risk You Haven’t Heard Enough AboutIn the world of integrative health, we look at the risk-to-reward ratio. For these new Alzheimer’s treatments, that ratio is an ethical minefield. While the benefits are marginal, the risks are catastrophic.Patients on these infusion medications require constant, expensive MRI monitoring to watch for "serious complications." These include:
- Micro-bleeding: Small, localized hemorrhages in the brain.
- Full brain bleeding: Massively damaging events that can lead to death.
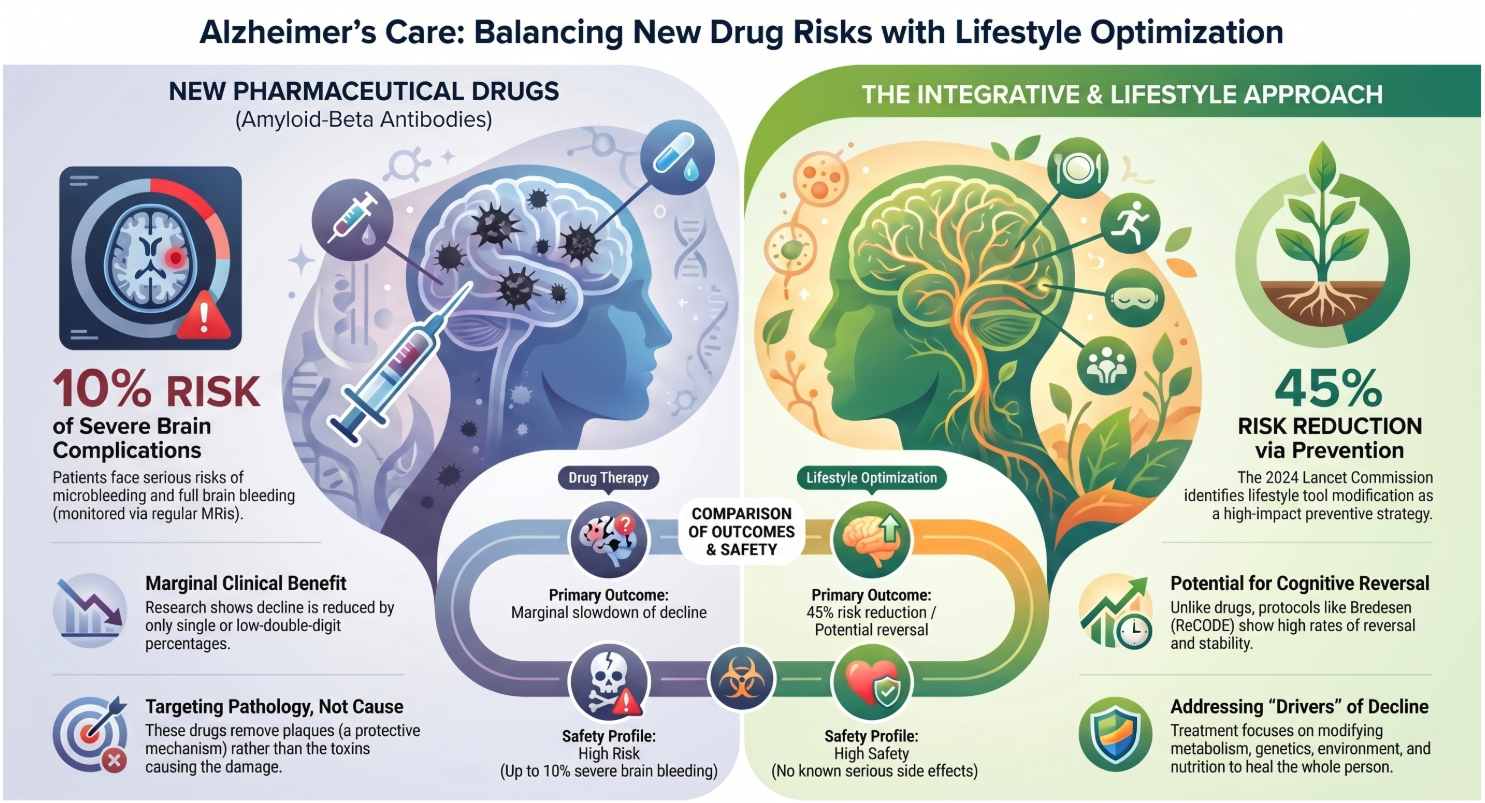
The risk for these catastrophic events can reach as high as 10%. This creates a profound ethical dilemma for doctors and families: is a single-digit percentage slowing of decline worth a 1-in-10 chance of a brain bleed? For many, the "hustle" and risk of the pharmaceutical approach simply do not justify the results.3. We Might Be Targeting the Wrong EnemyFor decades, the "amyloid hypothesis" has treated plaques and tangles as the villains of the story. However, emerging science suggests we’ve been attacking the brain’s defense system. There is a compelling theory that these plaques are actually protective mechanisms—the brain’s "vaults" used to sequester toxins and protect neurons.When drugs like Leqembi and Kisunla successfully clear these plaques, they may be inadvertently opening the vaults and releasing those sequestered toxins back into the brain. This explains the "Biomarker Gap": blood tests may show a "cleaner" brain with fewer plaques, yet the patient’s clinical condition fails to improve substantially. We are cleaning the pathology while ignoring the poison."Enough of treating pathology; it just doesn’t do anything. We have to work on the level of what causes the pathology, not the pathology itself." — 2024 Lancet Commission directive4. The Power of the "45% Factor"The 2024 Lancet Commission has shifted the conversation from pharmaceutical intervention to "drivers." Their research identified that 45% of dementia risk is tied to modifiable factors. This isn't just a marginal gain; it is a fundamental shift in how we view the disease.
| Treatment Type | Efficacy Detail | Clinical Outcome |
|---|---|---|
| Monoclonal Antibodies | Single-digit slowing of decline | Zero chance of reversal |
| Integrative Prevention | 45% risk reduction | Potential for stability |
| Integrative Programs | Full package of care (ReCODE/GWCIM) | Published cases of reversal |
To tap into this 45% reduction, we must move beyond the pill and address the primary drivers:
- Genetics: Understanding your unique predispositions.
- Environment: Identifying and removing the toxins the brain is trying to sequester.
- Metabolism: Optimizing internal chemistry to ensure the brain has the fuel it needs.
5. Reversal vs. Stability—The Integrative AlternativeWhile the pharmaceutical model offers zero chance of reversal, integrative programs are already achieving what was once thought impossible. Data from the Bredesen ReCODE trial and clinical experience at the GW Center for Integrative Medicine (GWCIM) show substantially stronger results than any drug currently on the market.This "full package of care" is a "true safe method" with no known serious side effects. Rather than high-risk infusions, this approach utilizes:
- Lifestyle Optimization: Tailoring daily habits to eliminate the "drivers" of decline.
- Nutritional Support: Providing the specific raw materials for cognitive repair.
- 40Hz Light Therapy: Using specific frequencies to stimulate brain activity and clearing.
The tragic irony is that while our medical system will pay for an infusion with a 10% risk of brain bleeding, it rarely covers the integrative protocols that offer a path toward reversal.Conclusion: Shifting the ParadigmThe future of Alzheimer’s care is not found in a laboratory-engineered antibody, but in a sophisticated understanding of the human ecosystem. We are at a turning point where we must stop "acting early" with the wrong tools and start "acting smartly" with the right ones.The evidence from the Cochrane Library and the Lancet Commission suggests that the pharmaceutical path is a short-lived hope facing a dead end. To truly protect our cognitive future, we must address the causes—metabolic, environmental, and genetic—rather than just cleaning up the debris they leave behind.This leaves us with a final, vital question: Do you view your brain health as a pharmaceutical problem to be managed, or a lifestyle ecosystem to be optimized?